Time for our monthly feature of a family who has endured a NICU stay with their baby.
Juanita and Nathan are kind enough to share the story of their son, Alexander.
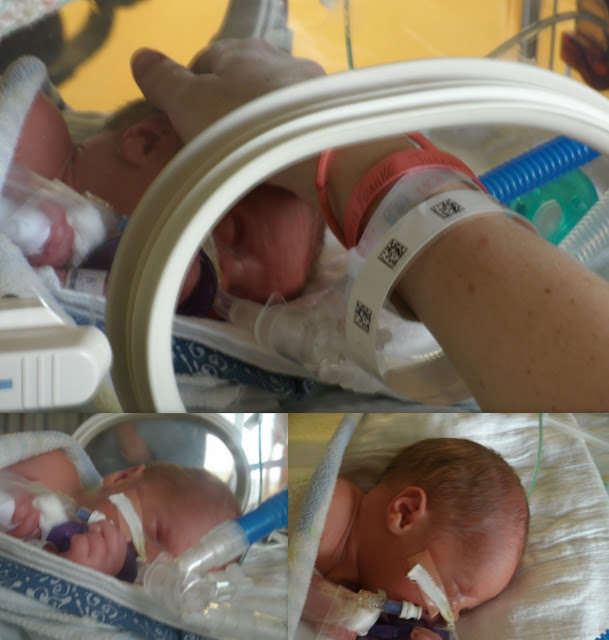
When I went into labor at 32 weeks, I was terrified. My previous son was born at 35 weeks, and everyone told me how lucky I was that he didn’t need to stay in the NICU. Unfortunately, his first year was a huge battle with breathing, eating, and eczema, and I didn’t want to repeat that battle. And the specter of the NICU loomed over this new son of ours.
After a traumatic cesarean delivery, Alexander was whisked away to the NICU while I went to the recovery room under general anesthesia. When I came out from under the anesthesia, I didn’t know how he was doing; I hadn’t even seen him yet.
After what felt like forever, I was wheeled up to the seventh floor to see my baby. And he was beautiful, all three pounds and seventeen inches of him. Of course, he was in the isolette, hooked up to all kinds of monitors, IVs, and a CPAP machine that was delivering a low dose of oxygen. His arms were the size of my middle finger, and his head was smaller than my palm.
That little miracle baby was mine.
While I was in the hospital for my own recovery, I was frequently in trouble with the nurses. My room was on the sixth floor, and Alexander’s was on the seventh, and I am still not sure why they thought I would leave him up there and stay in my bed. Of course, I spent as much time as I possibly could sitting next to the isolette, changing diapers, listening to rounds, and, of course, pumping breast milk for his feedings. Despite the fact that I could not hold my son for the first three days of his life, I wanted to be at his side as much as possible.
Because a baby born at 32 weeks hasn’t developed the sucking mechanism necessary for nursing, NICU moms have to pump breast milk that is then frozen in the hospital and used for future feedings. In fact, Alexander was initially given a substance called TPN, a mixture of proteins, carbohydrates, and lipids, through an IV because he couldn’t tolerate breast milk. It wasn’t until he was four days old that he started keeping his gavage feedings down. Gavage feeding is a little tube placed down the baby’s throat, and food is pushed down with a syringe. For three weeks, I was obsessed with how many milliliters of milk he was receiving and keeping down at each feeding.
All of the information I needed about Alexander—his weight, his temperature regulation, whether or not he’d had any “spells” of apnea or bradycardia, and his feeding volume—was given to me at morning rounds. The primary neonatologist, a resident, and several interns doing a NICU rotation would all come into the room and discuss Alexander. They would evaluate the data, ask me if I had any questions, and then explain their treatment plan for him. This process helped me piece together a lot of what was going on, and I made it a point never to miss rounds.
Aside from morning rounds, the saving grace of Alexander’s time in the NICU was “kangaroo time.” This is time when the baby and parent spend time cuddling skin-to-skin. Studies have shown that kangaroo time helps babies regulate their body temperature and mature faster. Medical studies aside, it provided a healing time for me and Alexander, and I spent each day looking forward to the next time I got to hold my son.
Once I was discharged from the hospital, our family got into a rhythm. My husband or mother would drive me to the hospital each morning, so that I could be there for rounds, morning cares, and kangaroo time. I would then go home to prepare lunch for my two other children, put them down for naps, and then do the dinner and bedtime routine. After that, my husband and I would return to the hospital for evening cares. I felt like I had my heart in two places at once, and my body was always in the wrong location. When I was not at the hospital, I worried about Alexander, and when I was at the hospital, I worried about the other two children.
While our stay at the NICU was brief, it was a very intense period, and I’m still not able to drive by the hospital and see Alexander’s window on the seventh floor. He just turned one last month, and he is doing better that I could ever have imagined. I am grateful to the doctors and nurses who cared for my son when I couldn’t, and I am so grateful to God for the miracle that is my young Alexander.
